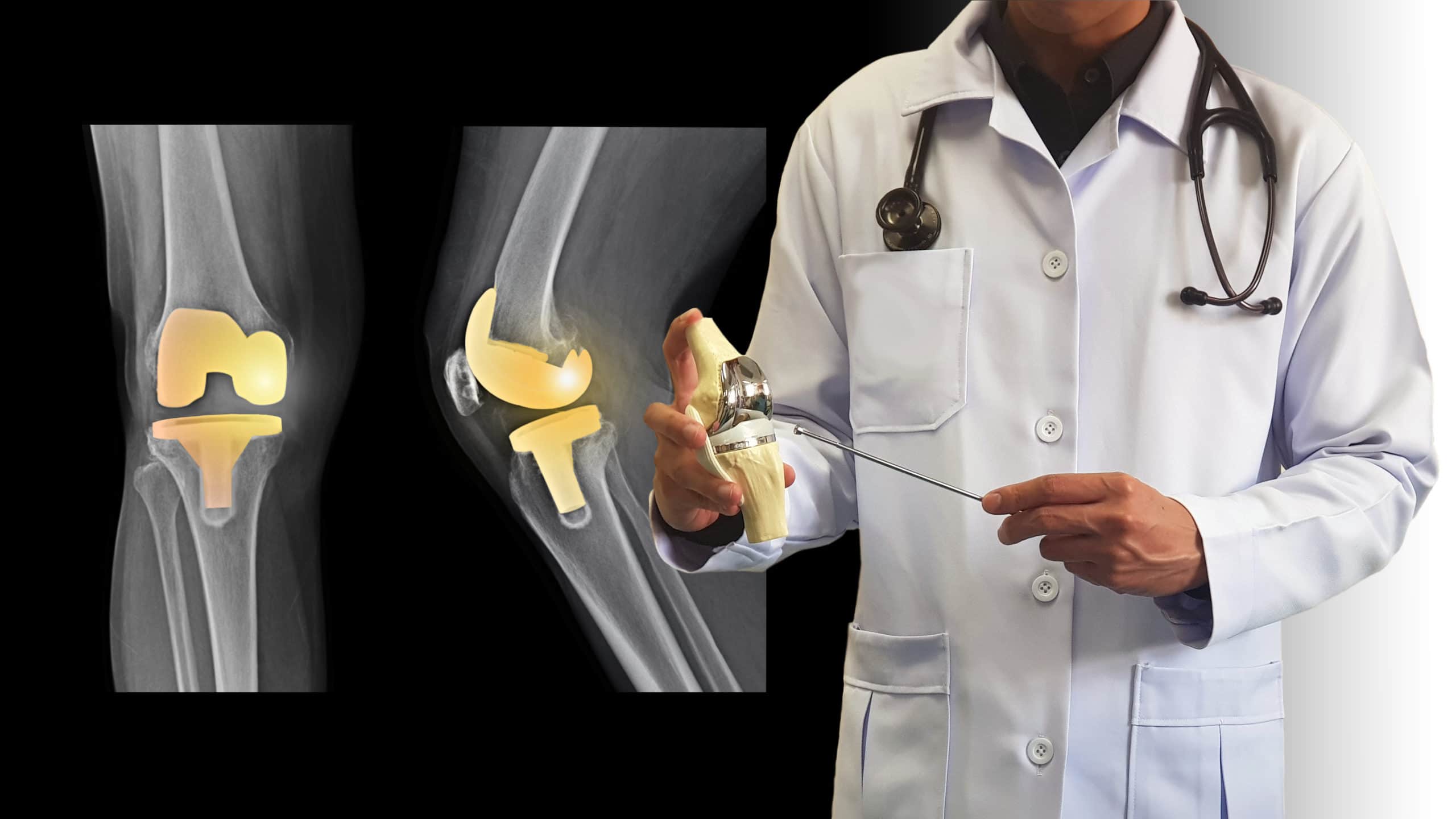
What is Arthroplasty?
Arthroplasty is the medical term that describes partial or complete joint replacements. In some cases, the procedure involves the resurfacing of a damaged joint structure. For some patients, it is necessary to replace the natural structure with an artificial joint (prosthesis).
It is believed that at least half a million arthroplasty procedures are currently performed in our country. Most of these procedures are performed on the knee and hip. However, arthroplasty may also be done to repair damage to a shoulder, elbow, ankle, or finger.
When is Arthroplasty Needed?
Joint replacement may be needed when a joint has been degraded by osteoarthritis. A joint may become arthritic as a result of a previous injury or due to wear and tear. Osteoarthritis is a condition in which the cartilage in a joint gradually breaks down. The thinning and fraying of cartilage can close the space between two bones that meet in the joint space, resulting in friction and deterioration of the bone. Arthroplasty is considered a last resort, planned when conservative therapies like medication and physical therapy no longer provide sufficient relief and mobility.
What Are Some Signs or Symptoms That Someone Might Need an Arthroplasty?
Many patients can mistake common symptoms for signs of aging when it comes to joint pain or osteoarthritis. However, constant, worsening symptoms, especially while doing simple physical activities, may be a sign of joint pain that may require treatment. These symptoms can include:
- Pain with a simple movement
- Stiffness
- Tenderness
- Loss of flexibility
- Bone spurs
- Swelling
- Redness
Who Is Most Prone to Developing Joint Issues or Osteoarthritis?
Joint issues and osteoarthritis can be common in people who are over the age of 50. If you are overweight, obese, or have a family history of joint pain, you may be at an increased risk for developing osteoarthritis and may need an arthroplasty if you leave your symptoms untreated. Chronic joint pain may also affect people who have previously sustained injuries to a joint.
Who Is the Ideal Candidate for Arthroplasty?
Ideal candidates for arthroplasty are adults experiencing severe joint pain or arthritis symptoms that no longer respond to anti-inflammatory medications. If your joint pain significantly impacts your quality of life or ability to do simple everyday tasks, you may benefit from an arthroplasty procedure.
However, if you are suffering from an active infection or have other underlying health conditions that may complicate your surgery, you may not be a suitable candidate for arthroplasty. Patients who are interested in arthroplasty but are still smokers should plan to quit several weeks before their procedure.
Are There Any Risks?
Like all surgical procedures, arthroplasty carries risks such as adverse reactions to anesthesia, infection, bleeding, and blood clots. A comprehensive consultation and examination are conducted to determine each patient’s risks based on their general health. Those who are immune-compromised, diabetic, or have heart problems tend to have higher risks for surgical complications. A surgeon can navigate these risks with various techniques and medications, such as blood thinners or antibiotics.
Nerve injury is a risk associated with surgery, though this is rare. After arthroplasty, there is a risk that the new joint may feel stiff or weak. This risk can be decreased by participating in the recommended rehabilitation following surgery.
What to Expect During Arthroplasty Surgery
Arthroplasty surgery is usually performed as an inpatient procedure. Patients may be in the hospital for a few days following their joint replacement.
The surgical procedure can take up to a few hours. Most arthroplasties are now performed using minimally invasive techniques. This shortens the length of incisions in most cases. The procedure involves either repairing or replacing the damaged part of the joint. For example, some arthroplasties involve replacing ball-and-socket structures with a biocompatible prosthesis. Once the joint has been repaired, the incision is closed with surgical staples or stitches. A bandage is placed over the incisions and the patient is moved to a recovery area where they are observed for a time.
What Is Recovery Like?
While still in the hospital, patients are seen by a physical therapist who will discuss their rehabilitation plan. Prescription medication controls comfort so well that patients can expect to be up and moving right away after their procedure. A walker, cane, or crutches prevents too much stress being placed on the repaired joint. At discharge, patients receive detailed post-operative instructions that outline how to care for their incisions.
Physical therapy may begin a day or two after discharge, if not while the patient is still in the hospital. The prescribed rehabilitation program helps patients resume normal activity and may continue for several weeks.
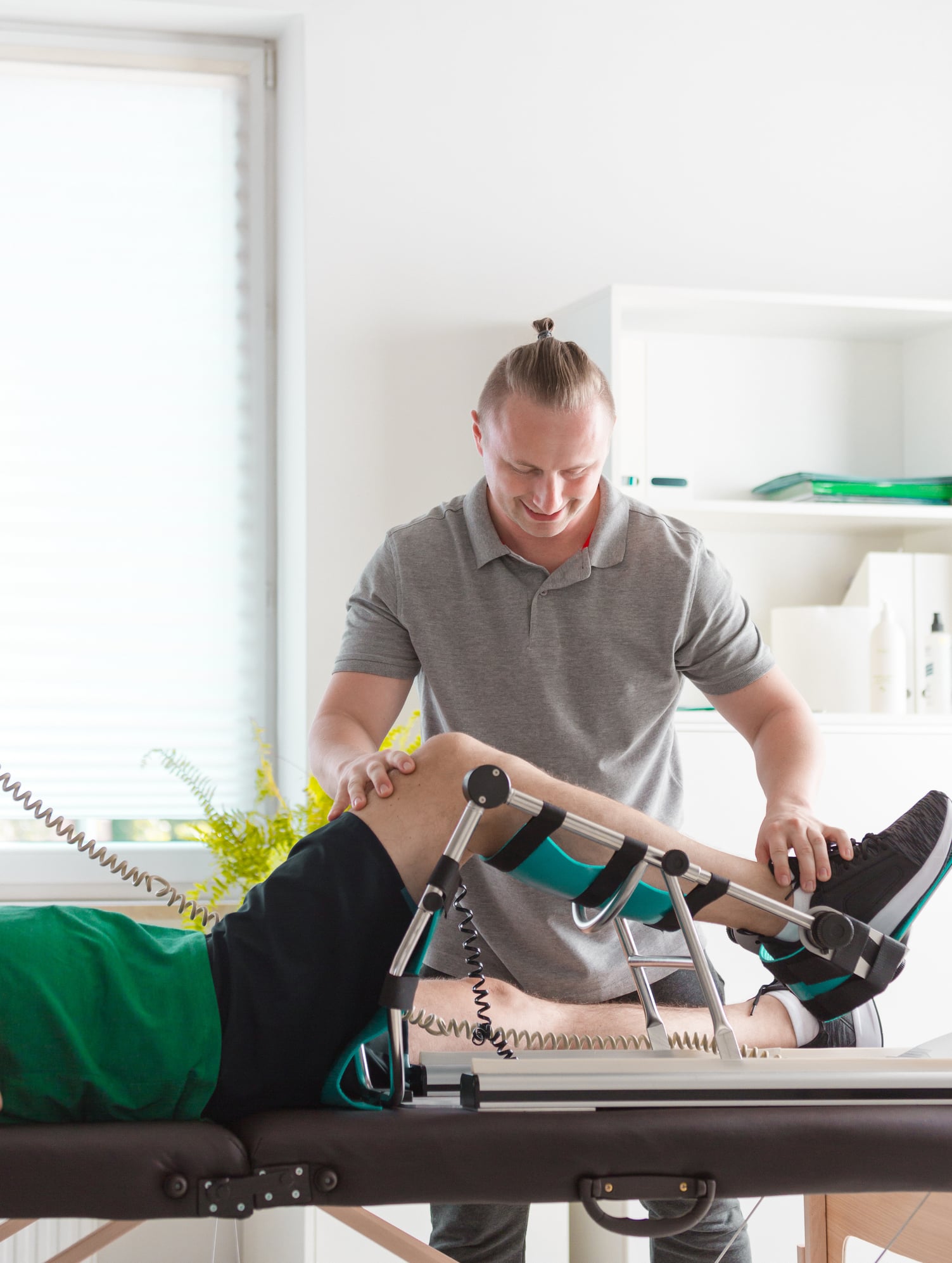
Improvements in strength, flexibility, mobility, and comfort occur each week that the patient continues to heal. A follow-up visit is usually scheduled for six to twelve weeks, or both, after surgery. At these visits, the surgeon can assess the progress that has been made and clear the patient for various activities.
What Happens If You Leave Joint Pain or Osteoarthritis Untreated?
While joint pain and osteoarthritis are not life-threatening conditions, they can be a major cause of pain and discomfort in a patient’s life. From impacting your ability to do simple movements like sitting or standing to experiencing chronic pain, untreated arthritis can severely worsen over time. For patients who experience severe arthritis symptoms, we recommend scheduling an appointment to determine your eligibility for arthroplasty as soon as possible.
Is Arthroplasty Covered by Insurance?
Each insurance provider may have specific qualifications for patients needing arthroplasty. When deemed medically necessary, covering is typically available for this procedure. Patients are advised to contact their insurance carrier directly for specific information related to their plan.
Read What Our Patients Are Saying!
"Very respectful and very quick in there service. Visit lasted no more then 35 minutes. Very professional."
Click here to read more reviews.
Schedule a Consultation Today!
For more information or to schedule you’re a consultation to discuss the joint replacement with one of our physicians, call us at 631.689.6698 or fill out one of our online contact forms and we will reach out to you as soon as possible.