Our bodies have an innate ability to heal themselves. However, with many injuries, there is not a proper environment to allow healing. Orthobiologics treatments involve the use of a patient’s own cells to facilitate healing, decrease pain and improve function. Common orthobiologic procedures include Platelet Rich Plasma (PRP) and cell therapies such as Bone Marrow Aspirate (BMA).
Orthobiologics aim to create a more favorable healing environment in the injured area of the body. The healing growth factors which naturally exist in our body’s blood and bone marrow are injected into the injured area. These cells can change the environment into one which optimizes healing with a more native cell type. Of course, the concentration of the different types of cells must be carefully determined by the orthobiologics specialist, as each location and type of injury requires specific formulation.
Orthobiologics can be used to treat a diverse range of orthopedic and sports injuries, both acute and chronic. This includes potentially repairing damaged tissues such as muscle, tendons, ligaments, and cartilage, as well as reducing osteoarthritis pain and improving mobility.
Benefits of Orthobiologics
Our bodies have amazing healing abilities. Orthobiologics rely on those processes to help the body heal itself. The goal of orthobiologics treatments in orthopedics is to facilitate tissue healing, decrease pain and improve function by using cells from the patient’s own body. This will return normal function and reduce or eliminate pain.
Some benefits of using orthobiologics for your orthopedic recovery include:
- Improve injury recovery.
- Repair damaged tissues.
- Reduce pain levels.
- Improve function.

Candidates for a Orthobiologic Treatment at Orthopedic Associates of Long Island
Orthobiologic treatments are used to treat the following conditions:
- Tendon injuries, including tendinopathies (tennis or golfer’s
elbow) and partial tears - Osteoarthritis
- Cartilage injuries
- Ligament injuries
- Plantar fasciitis
- Muscle strains
- and many others
What is Platelet-Rich Plasma?
Our blood has three types of cells: red blood cells that carry oxygen to the body, white blood cells that fight infection, and platelets that help blood clot and work to heal injuries. Plasma is the fluid part of our blood.
Platelets play an important role in healing wounds. Platelets are commonly known for their ability to clot the blood and close the wound, but they have a far greater role in healing than simply clotting. Platelets also house numerous growth factors, which are released to kick start the healing process of rebuilding the injured tissue.
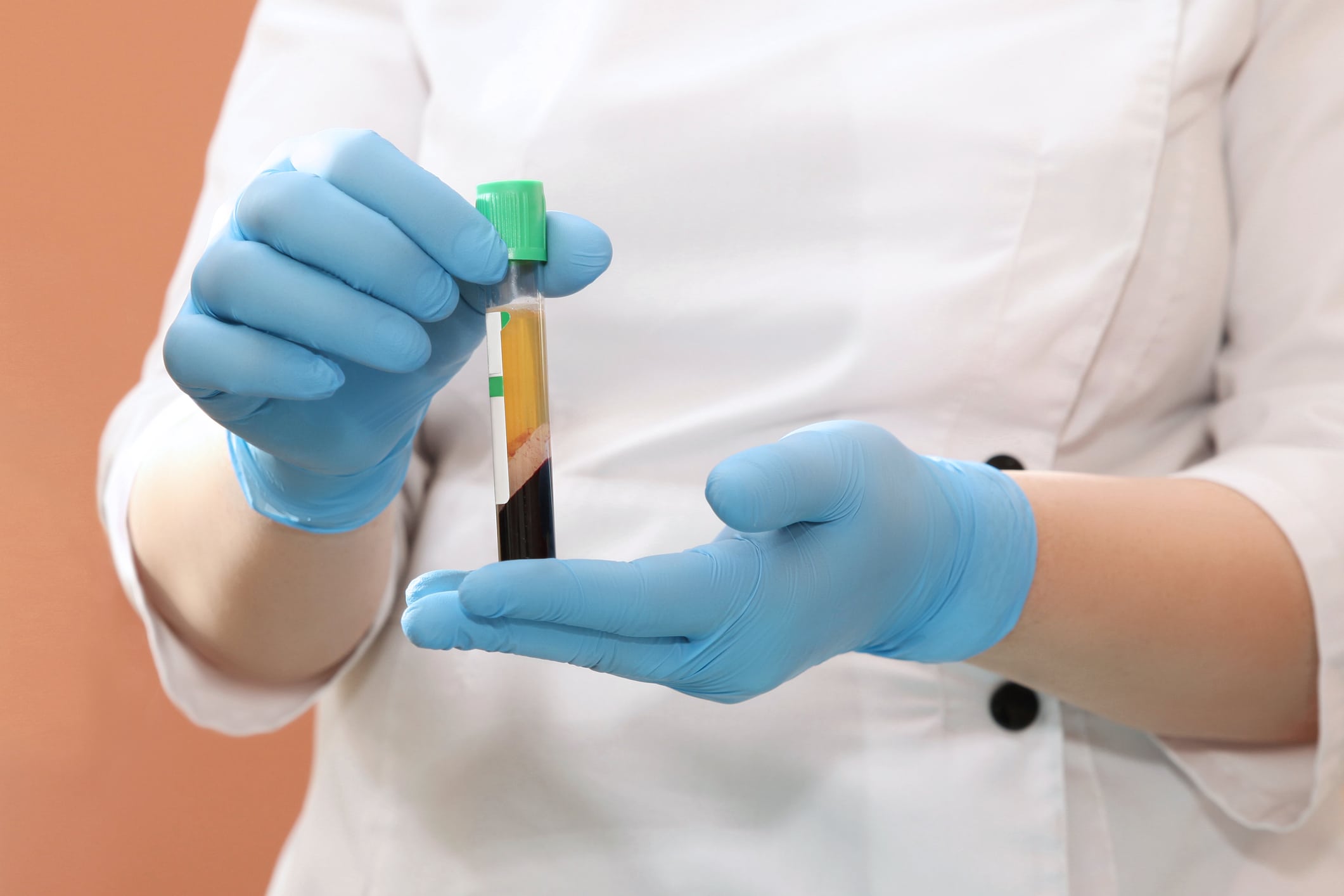
Centrifugation allows every sample of blood and its components to be specifically tailored to the needs of every individual patient and their specific injury.
How Does PRP Work?
When you have a wound or injury, such as a strained ligament, the body sends platelets to the area. With wounds, the platelets first form the clot to prevent more bleeding. Platelets then create a foundation for new tissue to grow. They also release growth factors and other proteins. These proteins attract stem cells and other cells to the area. All of these various cells, proteins, and growth factors work together to rebuild the injured tissue to fully heal and repair the injury
Concentrating platelets and their corresponding growth factors into PRP can elevate the healing potential. When concentrated PRP is injected into the injured areas, its acts like glue, binding the damaged tissue together. The PRP also releases growth factors that stimulate the body’s natural healing response.
How is Platelet-Rich Plasma Made?
Blood is drawn and then processed in a centrifuge to separate the cellular components. Depending on the condition being treated, the PRP will be formulated with different percentages of its components and then injected into the site of the injury.
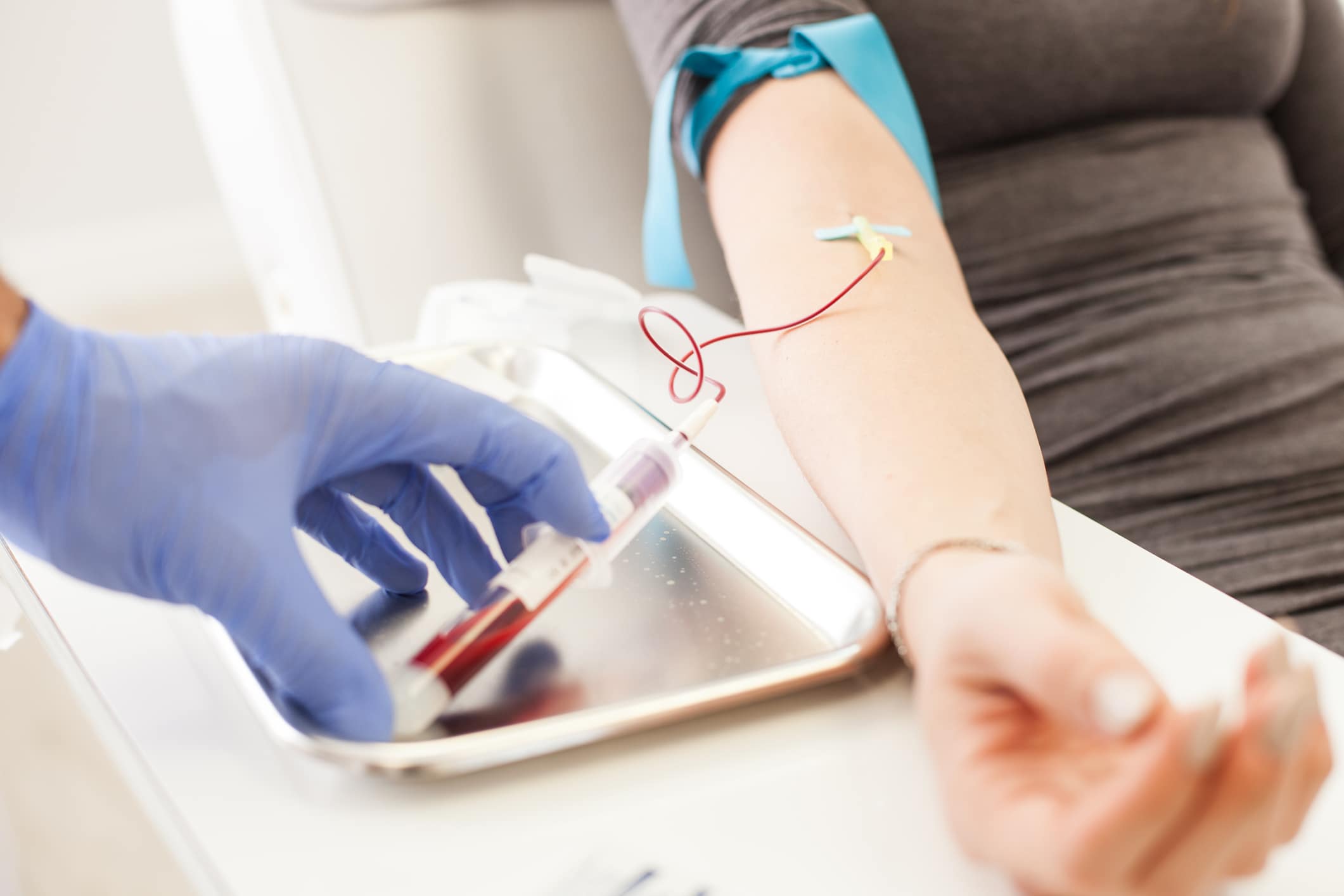
What is Bone Marrow Aspirate?
Bone marrow is the tissue inside our bones. It is responsible for most cell lineages including our blood cells which are made in the bone marrow. Bone marrow has stem cells and many other cells that help in healing. When you have an injury or illness, these cells help tissue heal and regenerate. The idea is that cells found in bone marrow can be used to treat damaged tissue, improve function, and help reduce pain.
How is the Bone Marrow Aspirated?
Bone marrow aspirate uses bone marrow that is harvested from the back of your pelvic bone. The process takes from 30 to 60 minutes. The procedure is completed with the patient on their side or stomach. Here are the steps of the BMA procedure:
- The harvest site on the pelvic bone is identified by touch and ultrasound.
- The skin is disinfected.
- A local anesthetic is applied from the surface skin down to the bone.
- A special needle is used to enter the bone.
- The needle withdraws (aspirates) the marrow from the bone.
- The bone marrow may or may not be placed in a centrifuge upon aspiration, depending on the procedure being performed.
Risks and Side Effects of Orthobiologics
After the orthobiologics treatment, there can be increased pain and soreness for a few days. As with any injection or procedure, there is a small risk of infection. There is also a small chance of developing a collection of blood called a hematoma around the harvesting site. This can cause pain and soreness, but typically resolves quickly. Since a patient’s own cells are used for the procedure, there is generally no allergic response or rejection of the treatment by their bodies.
What Our Clients Are Saying
“My previous surgeon notched my surgery and was lost. Dr. Gamez came to the rescue. You could NOT be in better hands. The only thing that matches his surgical skills, is his pleasant, truly caring demeanor. I can not recommend him any higher. You are in GREAT HANDS.” – Tom Brown
“I love Dr. Poupolo’s office all around!! Dr. Poupolo is AMAZING, he is always friendly and outgoing. Both my husband and I have had multiple surgeries with him and have had amazing recoveries. Also, his bedside manner is top notch always cheerful and friendly. He always lets you know what’s happening and tries to keep you unworried. He is also always looking for a way to help you with your ailment at your own pace and isn’t pushy for surgery. His physician assistants Tim and Matt are great, knowledgeable, and a pleasure when I am seen by them. I love Angela, I believe she is his medical assistant. I enjoy every time I go into the office no bad words to say about them.” – Kelly Adamski
Schedule a Consultation Today!
If you're interested in learning more about orthobiologics, please contact us for a consultation at 631.689.6698 or fill out our contact us form here. We will discuss your needs and concerns, and determine your best course of action.